On the COVID-19 Front Lines With 3 Allegheny Alumni
Health-care professionals share their stories about coping day-to-day with the global pandemic
As a front-line physician working in a hospital’s emergency room in Tennessee, Colleen Tran is focused on preserving the health and welfare of her patients, some of them very sick and facing a fight for their lives. The same is true for Lauren Moore, an emergency medicine resident in a Columbus, Ohio, hospital.
Jessica Schindelar is concerned with protecting and ensuring the safety of health-care workers like Moore and Tran. Schindelar is a member of the Centers for Disease Control and Prevention’s (CDC) COVID-19 Health Systems and Worker Safety Task Force.
All three health-care professionals are Allegheny College graduates. Their missions are similar during the current global health pandemic — to defeat the scourge of the novel coronavirus.
“I can truly say that I, probably like most of us, never expected to be in the throws of a pandemic let alone have my hands on the people infected with it every day,” said Moore. “It has absolutely brought a new admiration and appreciation for my colleagues and to all of the nurses, sanitation workers, respiratory therapists, medical techs, grocery store employees, and veterinarians, who, despite the risk, still willingly expose themselves to a deadly virus every day.”
These three dedicated health-care professionals took time from their hectic schedules recently to discuss their roles during the COVID-19 crisis.
Colleen Zink Tran ’07, Emergency Room Physician
Tran is an emergency room physician at TriStar StoneCrest Medical Center in Smyrna, Tennessee, a suburb of Nashville. She also serves as the assistant medical director for the emergency department. Every day since early March, her main duties have been the same.
“We are monitoring the positive cases and deaths daily,” Tran said. “We are testing symptomatic and asymptomatic patients in an effort to identify positive cases and quarantine to prevent spread. In preparation for a possible surge of patients, our hospital had set up tents outside where we would be able to rapidly evaluate patients that have symptoms concerning for COVID-19.”

The past two months have been a new learning experience for Tran, who graduated from Allegheny with a major in biochemistry and a minor in Spanish in 2007. “Life at work is very different from our usual. Normally, I would arrive at work in personal scrubs, log onto the computer, and start seeing patients. With this virus being so contagious, I now have many more steps to complete before starting my shift,” said Tran.
First, she gets her temperature checked upon entering the facility. If someone has a fever, they are sent home immediately and put on quarantine, she said. Tran then changes into hospital scrubs that are left at the hospital after her previous shift so it reduces the chance that she will bring the virus home on her clothing.
She picks up her masks — which include a simple mask for droplet protection and an N95 mask that is used during procedures such as intubation (putting a breathing tube down a patient’s throat) — and a face shield for the day. She scrubs her hands and arms up to her elbows with soap and water for 20 seconds to ensure that is not bringing in any of the virus. Lastly, she uses an antiviral/antibacterial wipe to clean off her computer, desk, chair, and anything else she may touch during her shift. Finally, she can log onto her computer and start seeing patients. At the end of her shift, the process is reversed, she said.
“In regards to the pathology I am seeing, there is definitely an increase in acuity or how sick patients are,” Tran said. “We are seeing many severely ill patients with difficulty breathing or with significantly low oxygen levels. These patients seem to get worse very fast and often end up on a ventilator. We have to take many precautions to not catch the virus while seeing these patients and especially while doing procedures on them, as this is when the virus can become airborne. For every patient who has symptoms of COVID-19, we have to wear a mask, goggles, a face shield, hair cover, gown, and gloves. This is very time consuming, so every patient I am seeing takes much more time than usual.”

Tran said her Allegheny education plays an integral role in her duties as an emergency room physician. “My time at Allegheny taught me critical thinking, time management, and how to be a leader. As an emergency physician, I have to be able to react quickly and often have to make hard decisions with minimal information. In the most stressful cases I have to be a leader for the staff and communicate my thought process,” she said.
Tran is married to a physician and has two children at home. Lately, when she gets home, she has been self isolating. “I try very hard not to touch my face and wash my hands often, even when at home,” Tran said. “I am taking daily zinc and vitamin C supplements as well. I am also focusing on my mental health and happiness in order to decrease stress. I try to separate my work life from my home life in order to avoid burnout, which is a common problem for emergency physicians.”
According to Tran, who earned her medical degree from Lake Erie College of Osteopathic Medicine, the toughest aspect of the COVID-19 outbreak has been to manage the anxiety, fear, and misunderstanding of the disease.
“It is frustrating to hear others minimize the virus, when I am risking my life by potentially exposing myself,” she said. “As the assistant medical director, it was initially very hard to calm my staff and the other physicians. Everyone was panicked that we may run out of masks or gowns. When this all started, there was a very steep learning curve as to how to protect yourself and we were getting conflicting advice daily. That was incredibly frustrating because we still wanted and needed to take care of our patients, but we wanted to protect ourselves as well.”
Watch this video to learn more about how Allegheny helped prepare Colleen Tran to fight COVID-19.
Jessica Schindelar ’02, Centers for Disease Control and Prevention, COVID-19 Health Systems and Worker Safety Task Force Communication Lead
Schindelar, the associate director for communication in the CDC’s Division of Healthcare Quality Promotion, is currently serving as the communication lead for the Health Systems and Worker Safety Task Force within the CDC’s COVID-19 response. She has been in this role since late March 2020 but has been working on the response since the end of January. She leads a team of 15 communicators from across the agency to translate the work of the task force through various communications channels to disseminate accurate, consistent, and clear COVID-19 information to key audiences and stakeholders, such as the nation’s health care workers.

Some of the important work of the task force is developing evidence-based guidance, recommendations, resources, and tools to protect healthcare workers and minimize the impacts of COVID-19 on the U.S. healthcare system. Some of the key issues she is working on are healthcare worker safety and infection control practices in healthcare settings, personal protective equipment, healthcare facility preparedness, and system-wide impacts.
“Our task force also provides technical assistance — both by deploying teams of experts to provide on-site assistance and providing remote assistance to healthcare facilities throughout the country, including nursing homes and long-term care facilities, which we are finding to be particularly vulnerable to COVID-19 outbreaks,” said Schindelar, who is a 2002 Allegheny graduate who majored in neuroscience and minored in art history.
Schindelar’s team is developing communication strategies and crafting important messages, creating fact sheets and toolkits, fielding interview requests from media, scripting and editing videos, and managing 60-plus web pages with critical and continually changing information for healthcare providers and facilities. The group is also writing social media, responding to questions from the public and professional audiences, hosting webinars and regular calls with clinical audiences and healthcare sector partners, and ensuring that the guidance and resources being developed by the task force are getting into the hands of the people that need them.
“I always felt like my neuroscience and art history combination was a bit of an odd one, but working as a public health communicator on healthcare safety issues has been a really lovely marriage of my interests in science and the arts,” said Schindelar. “I am forever grateful for my Allegheny education because it made me a better writer — this work requires that I’m clear and direct in my communications. I’m able to translate the scientific, technical information and guidance that is being developed by our task force into actionable messages and communication products that are easy to understand and use.
“Allegheny also armed me with the critical thinking and problem-solving skills I need to be successful in this kind of role — skills I am using every day when decisions have to be made in a split-second, sometimes with very limited information. Outside of my education, my Allegheny experience as a whole made me a stronger, more confident leader,” she said.
Schindelar said she has been following her own CDC guidance to protect herself: Staying home as much as possible, frequent handwashing, practicing social distancing, and wearing a face covering to protect others when she goes out to run essential errands — which is mostly just grocery store runs, she said. Generally, she tries to get enough sleep, eat healthy, and take walks in her neighborhood to get in exercise to counterbalance the hours she works.
“There are two things I am finding particularly tough during this crisis,” said Schindelar. “First, is hearing from friends, former classmates, and other healthcare workers who are on the front lines about the challenges they are experiencing. It’s difficult to hear the realities about what is happening on the ground, and I am so grateful for everything they are doing. I am trying to do my part to help them — as are the more than 4,000 CDC staff working around the clock on this response to protect the public’s health. Seeing the dedication and commitment of the 300-plus people within my own task force who I’m working with every day to protect healthcare workers and facilities makes me really proud to be part of this historic response, even on the hardest days.”
The second challenge is that the CDC staff is mostly running this response from their homes, she said. “There is a skeleton crew at CDC right now. Before we moved to remote work in March, our emergency response operations happened out of two buildings on CDC’s campus — we were all working out of our task force ‘war’ rooms. That is all happening virtually now, and while I feel very fortunate that I can do this work from the safety of my own home, many of my colleagues are now juggling this response with childcare and school as well. It’s an added layer of difficulty we’ve never encountered in any response I’ve been involved with in my 12 years at the agency. But in the end, it’s rewarding work despite the long hours and I go to bed every night really proud of the work we have done and are doing.”
Lauren Moore ’14, Emergency Medicine Resident
Moore is a postgraduate year two emergency medicine resident at The Ohio State University Wexner Medical Center. She is nearing the end of her second of three years of post-medical school training. “We see everyone — the deathly sick, the not so sick, and all those in between, regardless of whether or not they have signs or symptoms of COVID-19,” Moore said.
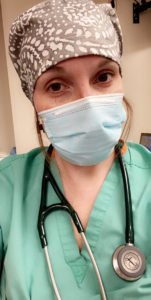
Successfully managing the crisis is all about delegating resources, she said. “This means that we have to determine what patients need further management and monitoring in the hospital versus who can safely go home. Aside from life-saving care, we provide public information, resources, and a hand to hold during this uncertain time. I’m honored and privileged to be able to do this as my job,” Moore said.
“From a hospital standpoint, policies change based on new data at a rate of what seems like two to four times a day. We have to keep up with ever-changing COVID-19 testing kits, sanitation practices, who to test and how to keep safe,” said Moore, who is a 2014 Allegheny graduate and a 2018 graduate of the Penn State College of Medicine.
Additionally, she said, the Wexner Medical Center emergency room is seeing a “backlash from the pandemic.” Because so many people are cooped up at home, there has been an increase in the number of child abuse victims, domestic violence assaults and suicides, Moore said.
Also, hearing about colleagues and fellow first-line providers getting sick is disconcerting, Moore said. “Sometimes, when I’m driving home after a 12-hour shift, the weight of the situation hits me and I have to remind myself to take a deep breath and forge ahead,” Moore said. “It’s overwhelming. It’s like walking a tight rope on the sharp edge of a knife. On one side, we want to do right for and be there with our patients despite limited personal protection equipment and increased risk to ourselves. But on the other, we want to protect our families and friends. Either way we fall, in a lot of ways, we get cut.”

Earning a bachelor’s degree in neuroscience at Allegheny while taking all the necessary pre-med classes was tough, Moore said, but worth it. “Long hours of studying in Steffee to get into medical school prepared me for the academic workload of staying up to date with the ever-changing guidelines and research regarding best COVID-19 treatment practices. I was also very involved in student government, my sorority Kappa Kappa Gamma, and working at the childcare center, in Alumni Affairs at the Tippie Center, at the Office of Student Involvement, and as a health coach. Having so many commitments in addition to my studies prepared me for extreme multitasking, which is imperative to success in a busy emergency room and intensive care unit.”
While personal protective equipment has been limited during the pandemic, hospital management has done everything it can to make sure physicians and other workers are as protected as possible, Moore said.
“I don’t have a safe place to store my gear at the hospital, so I leave it in my car and have been avoiding using my car unless it is to get to work,” she said. “More importantly, I’m protecting my family and friends by staying away from them. I even sent my dog away for several months to protect the dog walkers who I rely on to help me with her. It may sound silly, but that to me has probably been one of the hardest things to deal with during all of this — not coming home to her company after a long day.”
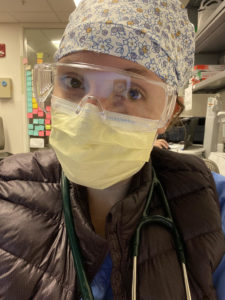
In an attempt to prevent viral spread and exposure to those whose bodies are already weak, visitation from the public is limited at Wexner Medical Center, as it is at all medical facilities now.
“Because of this, so many people are going through some of the most difficult times of their lives completely alone, and it’s tough to watch that,” Moore said. “Patients are brought in by EMS completely alone, and we put breathing tubes and IVs and catheters in them and they are so sick that they can’t even talk to their families on the phone to tell them what’s going on. When I provide phone updates to families, I find that it is equally as hard for them who want nothing more than to see and be there for their loved ones. All I can do is be there for the patients by holding their hands and reminding them that their families love them.”